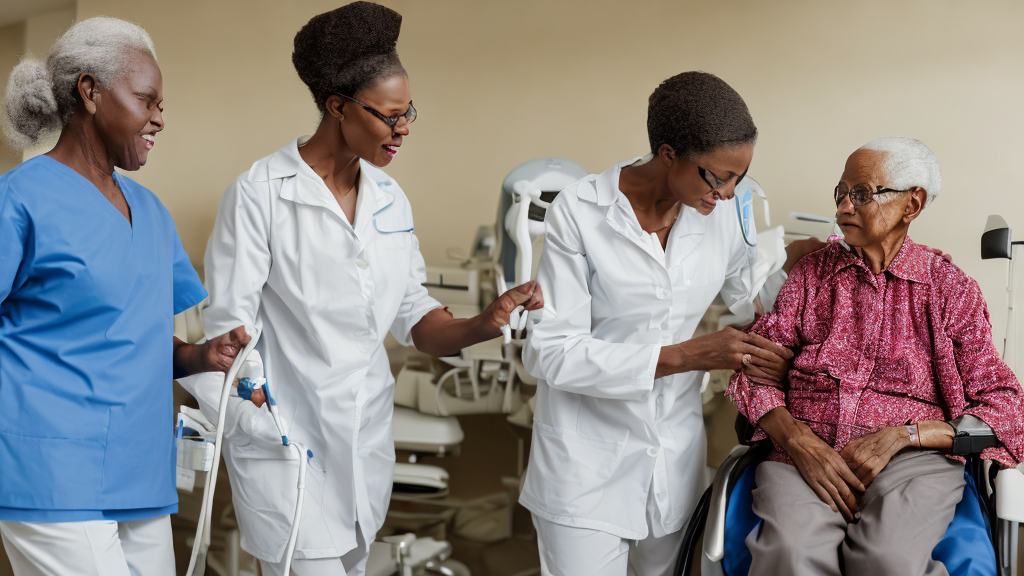Warfarin and newer direct oral anticoagulants require vigilant monitoring in eld...
Anticoagulation therapy — used to prevent and treat thromboembolic conditions including atrial fibrillation, deep vein thrombosis and pulmonary embolism — presents particular challenges in elderly patients. The pharmacokinetics of anticoagulants change with age, and the margin between therapeutic anticoagulation and dangerous haemorrhage narrows significantly. Falls, cognitive impairment and polypharmacy all compound this risk.
Warfarin requires regular INR monitoring and careful dose adjustment, and patients must be counselled on dietary interactions (particularly vitamin K intake) and the need to report any unusual bruising or bleeding promptly. The newer direct oral anticoagulants (DOACs) — including apixaban, rivaroxaban and dabigatran — are increasingly preferred for their predictable pharmacology and lack of routine monitoring requirements, but they still demand careful patient selection and adherence support.
Home care nurses play a vital role in anticoagulation management: reinforcing adherence, monitoring for bleeding signs (including hidden sources such as gastrointestinal bleeding indicated by dark stools), facilitating timely INR checks and communicating with the prescribing team regarding any changes in the patient's clinical status or new medications.